Where You Live May Be Linked To How Much Arthritis Pain You Experience
1 year ago
8621
0
Posted on Jul 21, 2023, 3 p.m.
In America the prevalence of moderate or severe joint pain due to arthritis varies significantly across the nation, ranging from 6.9% of the population in Minnesota to 23.1% of the population in West Virginia according to a new study published in the journal PAIN led by University at Buffalo The State University of New York.
Estimates are that around 59 million Americans (23.7%) are living with arthritis, and at least 15 million of those are experiencing severe joint pain related to that condition. Those with severe pain also face a diminished range of motion, disability, and mortality that is associated with the condition.
“The risk of joint pain is over three times higher in some states compared to others, with states in the South, especially the lower Mississippi Valley and southern Appalachia, having particularly high prevalence of joint pain,” says Rui Huang, a sociology Ph.D. student in the UB College of Arts and Sciences, and the paper’s first author. “We also observed educational disparities in joint pain in all states that vary substantially in magnitude, even after adjusting for demographic characteristics.”
Education may play a role as the percentage point difference between those who did not complete high school vs those who obtained at least a bachelor’s degree varies strikingly as well ranging from 31.1% in West Virginia to 29.7% in Arkansas, and 28.3% in Alabama to 8.8% in California, to 9.8% in Nevada to 10.1% in Utah.
“Education can function as a ‘personal firewall’ that protects more highly educated people from undesirable state-level contexts, while increasing the vulnerability of less educated individuals,” says Huang.
“Very little research has examined the geography of chronic pain, and virtually none has examined the role of state-level policies in shaping pain prevalence,” says Hanna Grol-Prokopczyk, Ph.D., UB associate professor of sociology, and a co-author of the study. “We were excited to identify state characteristics that reduce residents’ risk of pain.”
For this study, the combined data was analyzed on 407,938 people between the ages of 25-80 from the 2017 Behavioral Risk Factor Surveillance System with state-level data about SNAP programs (formerly known as food stamps), Earned Income Tax Credits, income inequality, social cohesion (relationship strength among community members), Medicaid Generosity Scores, and tobacco taxes.
SNAP programs exist in all states, but some offer more benefits to qualifying residents than others. States with more expansive and generous SNAP benefits were found to have a lower prevalence of pain, and this was also true for states with greater social cohesion which indicates that both social functioning and material resources play critical roles in shaping the risk of pain. The researchers suggest that this study provides information regarding pain disparities across the nation and may help to inspire renewed interest in research that puts equal emphasis on both macro and individual-level factors.
“The increase in the generosity of SNAP benefits could potentially alleviate pain by promoting healthier eating habits and alleviating the life stress associated with food insecurity,” says Huang. “Social factors such as conflict, isolation and devaluation are also among the ‘social threats’ that can lead to physical reactions such as inflammation and immune system changes.”
“Chronic pain can – and should – be addressed through macro-level policies, as well as through individual-level interventions,” says Huang. “This study also implies that pain research in general should move towards a greater understanding of the macro contextual factors that shape pain and pain inequalities.”
Controlling for various covariates the average prevalence of joint pain was 12.9% with the prevalence varying substantially in individual states. Prevalence was found to be the lowest in Minnesota at 6.9%, which was followed by 7.5% in Hawaii, and Utah with 7.7%. Prevalence was found to be the highest in West Virginia at 23.1%, which was followed by Alabama at 21.6%, and Arkansas with 21.4%. The researchers concluded that those living in high-prevalence states are more than three times more likely to experience joint pain than those living in low-prevalence states based on their findings.
The ten highest pain states were: West Virginia, Alabama, Arkansas, Kentucky, Mississippi, South Carolina, Tennessee, Oklahoma, Louisiana, and Michigan.
The ten lowest pain states were: North Dakota, Washington, South Dakota, Nebraska, Iowa, Alaska, Colorado, Utah, Hawaii, and Minnesota.
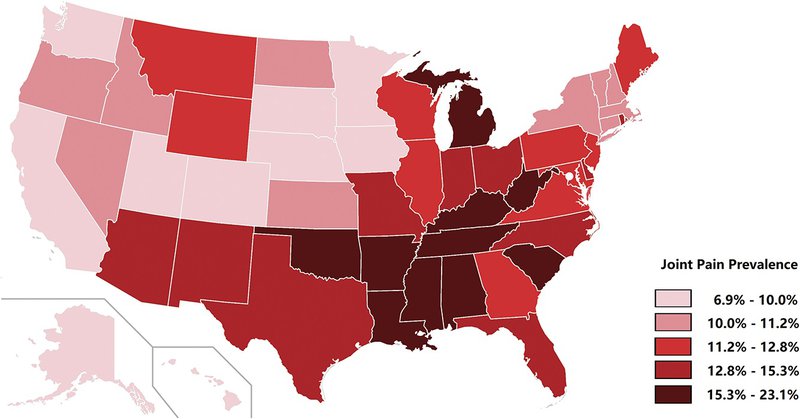
Image: Map of predicted probability of arthritis-attributable moderate/severe joint pain prevalence in adults aged 25 to 80 years, by state, adjusted for age and other demographic characteristics. Credit: Copyright © 2023 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of the International Association for the Study of Pain.Source PAIN: 7/03/2023
As with anything you read on the internet, this article should not be construed as medical advice; please talk to your doctor or primary care provider before changing your wellness routine. This article is not intended to provide a medical diagnosis, recommendation, treatment, or endorsement.
Content may be edited for style and length.
References/Sources/Materials provided by:
Rui Huang, Yulin Yang, Anna Zajacova, Zachary Zimmer, Yuhang Li, Hanna Grol-Prokopczyk. Educational disparities in joint pain within and across US states: do macro sociopolitical contexts matter? Pain, 2023; DOI: 10.1097/j.pain.0000000000002945
https://www.buffalo.edu/news/releases/2023/07/huang-joint-pain.html
https://cdn-links.lww.com/permalink/pain/b/pain_2023_05_02_huang_pain-d-22-01252_sdc1.pdf









