Can a MED Diet Rich In Olive Oil Be Healthy For Heart Patients?
1 year, 10 months ago
8678
0
Posted on Sep 07, 2022, 3 a.m.
Article courtesy of Dr. Joel Kahn, MD, who is a Clinical Professor of Medicine at Wayne State University School of Medicine, one of the world's top cardiologists, best-selling author, lecturer, and a leading expert in plant-based nutrition and holistic care.
What is the CORDIOPREV Study?
- The CORonary Diet Intervention with Olive oil and cardiovascular PREVention study (CORDIOPREV) is a single-center, randomized clinical trial aimed at assessing the superiority of a Mediterranean diet in the secondary prevention of cardiovascular disease (CVD), as compared with a lower fat diet.
How Did They Do the CORDIOPREV Study?
- The calculated sample size of 491 patients in each group was based on standard assumptions of rates of events in patients with known coronary artery disease (CAD) called secondary prevention.
What Patients Were in CORDIOPREV?
- The study population was made of 1002 patients (average age, 60 years; 83% males) with established coronary heart disease; 58% had metabolic syndrome with a body-mass index of 31 kg/m2, 54% had diabetes, and 68% were hypertensive. Lipid-lowering, antithrombotic, and anti-hypertensive drugs were taken by the vast majority of patients. They were clinically stable in the previous 6 months, and randomly assigned in a 1:1 ratio to receive a Mediterranean high olive oil diet or a lower fat diet, with a follow-up of 7 years. Extra-virgin olive oil and healthy low-fat food were provided to each subject assigned to the Mediterranean or lower-fat diet, respectively.
What Was In the 2 Diet Plans?
- The Mediterranean diet was modeled by prescribing 35% of the calories as fat (22% monounsaturated fatty acids) and a maximum of 50% carbohydrates, while the lower-fat diet comprised less than 30% of total fat (12–14% monounsaturated fatty acids), and a minimum of 55% carbohydrates. In both diets, the cholesterol content was adjusted to less than 300 mg per day and proteins provided 15% of energy. No energy restriction or physical activity was promoted. All patients received comprehensive, tailored, and continuous dietary support, with at least 12 interactions per year between dietitians and participants in order to keep them adherent to the nutritional plan.
Was There a Difference in Adherence to the 2 Diets?
- Baseline adherence of the whole population was better for the Mediterranean diet (8.8 on a 0–14 scale) than for the low-fat diet (3.8 on a 0–9 scale).
Was There a Difference in Outcome?
- After 198 primary-outcome events, the study was stopped: 87 (17.3%) occurred in the Mediterranean diet group (High Olive Oil) and 111 (22.2%) in the lower-fat group. The unadjusted hazard ratio was 0.75 or a 25% reduction in the high Olive Oil group. The Mediterranean diet was consistently superior to the low-fat diet in all multivariable-adjusted models. All components of the composite primary outcome were numerically, but not significantly, lower in the former than in the latter.
Implications?
In this large randomized study over 7 years in actual patients with heart disease, the lower-fat diet did not perform as well as the MED diet with added olive oil. Neither diet was fully plant-based (vegan) and neither diet was no-oil so it is unknown if either of these would have performed better. For the patient willing to change to the MED diet, additional olive oil is not harmful and may be helpful.
About the author: At his core, Dr. Joel Kahn believes that plant-based nutrition is the most powerful source of preventative medicine on the planet. Having practiced traditional cardiology since 1983, it was only after his own commitment to a plant-based vegan diet that he truly began to delve into the realm of non-traditional diagnostic tools, prevention tactics, and nutrition-based recovery protocols.
As with anything you read on the internet, this article should not be construed as medical advice; please talk to your doctor or primary care provider before changing your wellness routine.
Content may be edited for style and length.
Materials provided by:
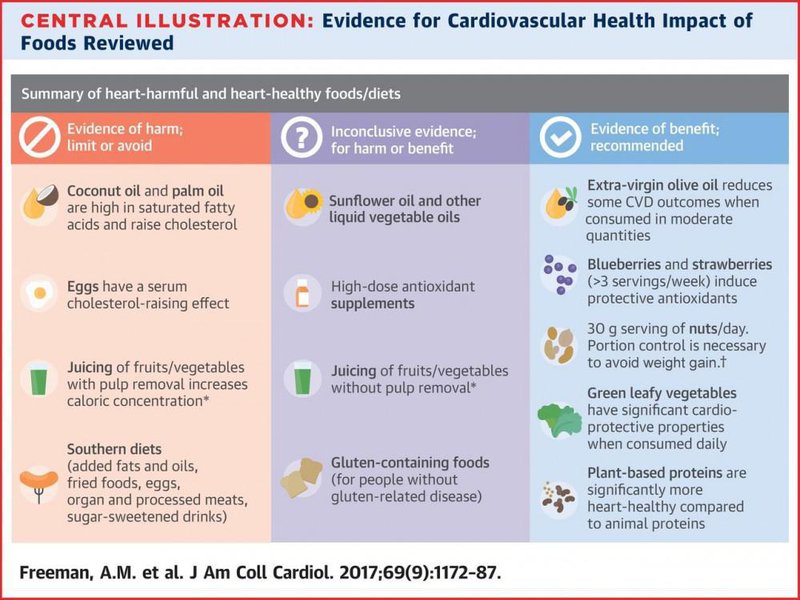
Image: Freeman, A.M. et al. J Am Coll Cardiol. 2017;69(9):1172-87









